
The biopsychosocial model of health is a unique approach to understanding the factors involved in the overall health, well-being, and healing of human beings. An alternative approach to the biomedical paradigm for assessing and understanding health, this model rejects the reductionist idea that the mind and body are separate.
The biopsychosocial approach was introduced by psychiatrist George Engel in the 1970s. Concerned about the difficulties facing psychiatry and mental illness at the time, Engel published a landmark paper suggesting the traditional biomedical model failed to consider the behavioral, psychological, and social dimensions of pain and illness.
He believed, in order for us to truly understand and nurture good health, we must first look beyond the sensory modalities and neurological components of pain. Engel suggests pain and illness are a result of dynamic interactions between a multitude of different factors in our lives. In other words, pain isn’t just a perceptual phenomenon, but a result of a disruption in the body’s homeostatic systems.
Doctors and healthcare providers pursuing the biopsychosocial model of health recognize how we feel physically, and how the systems of our bodies work are dependent not just on our physiology, but also our social situations and mental wellness. When applied correctly, the biopsychosocial model emphasizes the importance of maintaining good overall health in all aspects of our lives.
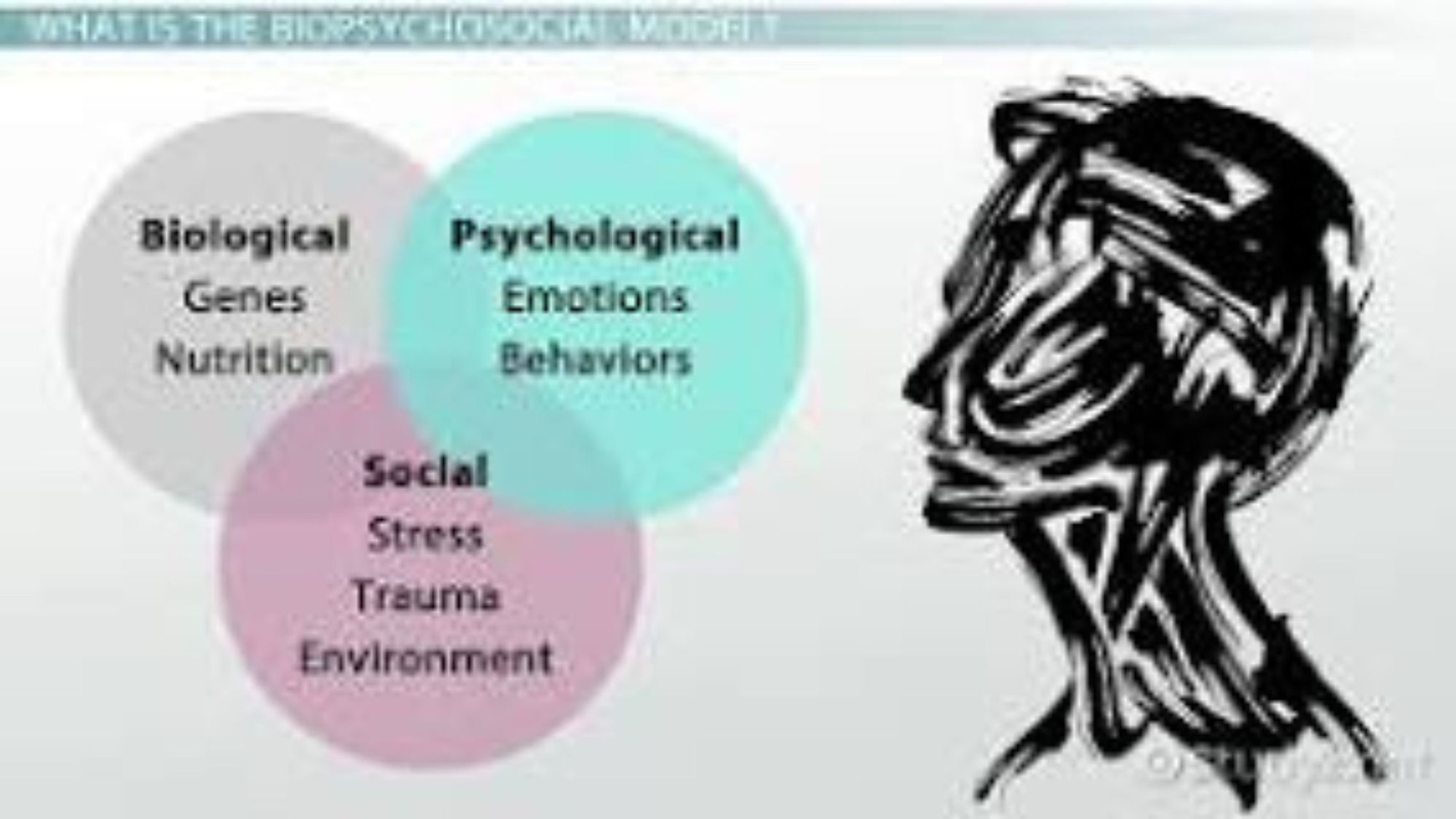
What is the Biopsychosocial Model of Health?
The biopsychosocial (BPS) model proposed by George Engel was introduced as an alternative to the traditional biomedical paradigm for health.
The biomedical model looks specifically at the physical components of illness. For example, if a patient was experiencing depression, a doctor following the biomedical model would look at potential changes in the individual’s brain chemistry to determine the cause of the problem, and create a potential treatment plan. The biopsychosocial approach encourages medical professionals to conduct a more complete assessment of how different components outside of biology can influence wellness. This includes social and environmental factors.
The biopsychosocial model emphasizes the connection between biological, psychological, and social-environmental factors in health.
This paradigm suggests a person may have a genetic predisposition for a condition, but they must also be exposed to other psychological and social factors to trigger the illness. In the case of depression, for instance, a person may have a history of mental health conditions in their family, but they may not experience depression until they encounter extreme stress at work or, for example, in toxic relationships.
Engel re-introduced the connection between the mind and body which had previously been overlooked by the biomedical approach.
Following Engel’s publication, the BPS model was embraced by the World Health Organization as a foundational basis for the International Classification of Function. This model has also inspired further research into the psychological and social components which may influence our health. For example, holistic health professionals now look at how spirituality and culture can affect wellbeing.
The Components of the Biopsychosocial Approach to Health
Fundamentally, the biopsychosocial model examines how biological, psychological, and social components play a collaborative part in health or disease.
The three core aspects examined in the biopsychosocial approach are:
· The Biological: The biopsychosocial approach still considers physical health as an important aspect in wellness. However, it indicates there’s more to wellbeing than biology. In some cases, biological concepts have the biggest part to play in a disease or illness. A person suffering from a hernia or cancer diagnosis may not be heavily influenced by their social or psychological situation.
· The Psychological: The BPS model also considers how mental and emotional wellness can influence behavior, and health. In many cases, our physical health can influence our mental health, and vice versa. A person with diabetes, for instance, may experience more severe symptoms such as fatigue and discomfort, caused by concern about their condition. Mental health issues can also influence how we address ailments, and whether we adhere to the recommendations given by doctors.
· The Social: Interpersonal factors, such as community experiences and social interactions can sometimes influence our wellness. Being isolated from people we care about can lead to feelings of depression and anxiety which worsen physical illness. During the pandemic, consistent isolation, among other factors, triggered a 25% increase in the prevalence of depression and anxiety cases worldwide.
The BPS model indicates relative disease and health is dependent on the interaction between all of the three factors listed above. The interplay of these components can determine the cause, and severity of an illness, as well as the symptoms exhibited by patients. Examining all three concepts can also help medical professionals to choose a more effective treatment path for patients.

How are Biopsychosocial Assessments Conducted?
Medical professionals following the BPS model often assess patients and their conditions with a more holistic approach. Rather than just looking at the physical symptoms and biological components of an illness or disease, practitioners attempt to explore the social and psychological factors which may be contributing to the condition as well.
Although there’s no definitive list of assessment or diagnostic methods to use with this approach, clinicians attempt to gain a deeper insight into the nature of the condition, asking questions about a person’s background, psychological symptoms, and social experiences.
For example, if an individual visits their doctor complaining of persistent headaches, the medical practitioner may start with a physical assessment, checking the patient’s eyes for visual issues, asking about their diet, and even conducting scans to check for signs of brain disturbances.
However, they would also ask the individual about their mental health, experiences with stress, and discuss the aspects of their daily routine.
Using this strategy of assessment, the medical practitioner can suggest a treatment approach which tackles all of the issues contributing to the ailment. This could involve suggesting glasses if a person has trouble with their vision which might be worsening the headaches. However, it could also mean connecting a patient with a therapist so they can learn how to reduce feelings of stress.
Practitioners using the BPS model know even if two patients are referred to a clinic with a matching diagnosis, they can differ psychologically, physically, and socially. Because of this, one-size-fits-all treatment methods are rarely used. Instead, treatments often revolve around:
· Education: Helping patients to understand how various mechanisms contributing to their pain or ailment could be influencing their symptoms, so they can address each issue. If a patient experiences worse headaches when at work, this could be related to feelings of increased stress or anxiety in the workplace.
· Symptom management: Similar to the biomedical model, the BPS approach also looks for ways to manage symptoms, using a multitude of different medications, self-care strategies, and support from professionals. Symptom management may include taking certain medications, seeking therapeutic treatment, or making alterations to a daily routine.
· Lifestyle strategies: The biopsychosocial model of treatment often includes making lifestyle changes intended to address the psychological and social aspects of illness. Doctors could recommend meditation for stress, counselling, or even changing a specific situation, such as seeking out an alternative form of employment.
Benefits of the Biopsychosocial Approach for Holistic Wellbeing
The biopsychosocial model of health takes a holistic approach to understanding and treating ailments. It acknowledges that episodes of poor mental health and difficult social situations can contribute to and exacerbate physical illness.
Studies have proven that patients experiencing severe stress and mental turmoil may have lowered immune systems and reduced healing mechanisms. As such, in order to fully recover from a physical ailment, patients may also need assistance managing social and psychological factors. A patient recovering from an injury, for instance, may need therapy to assist them in managing the challenges of their condition, as well as regular exposure to positive social interactions.
Similarly, the BPS model suggests a patient with a mental health condition, such as depression or anxiety, may also be at greater risk of illness. Conditions such as depression are frequently accompanied by inflammatory issues and immune system problems.
The biopsychosocial approach pushes practitioners to find ways of reducing a patient’s vulnerability to additional symptoms and worsening conditions in the long-term. If a medical professional was assessing a smoker from a biomedical perspective, they would look at their genetic reasons for smoking, such as having a more addictive personality.
However, a medical professional looking at a smoker from a BPS approach would consider the idea that people might start smoking for psychological reasons, such as stress, or social reasons, such as being surrounded by smokers on a regular basis. Assessing all potential contributing factors allows for the creation of a more comprehensive treatment model.
Looking at Health from a BPS Perspective
The biopsychosocial model teaches us there are often a number of contributing factors involved in any ailment or disease. The biological, social, and psychological factors in your life need to work together in harmony in order to preserve good health. When one of these aspects is disturbed, it can have a lasting negative effect on the others.
You could start looking at your own health and wellness circumstances from a biopsychosocial perspective, by examining your CircleDNA test results.
This at-home DNA test requires a simple cheek swab to give you health insights based on your unique DNA. You may find you have a higher risk of depression or obesity for example, due to your genetic makeup. However, you may also learn that your issues with self-esteem can increase your chances of eating unhealthy foods in larger quantities.
Similarly, you may discover that your behavior in social situations, such as eating at restaurants with others, or going drinking regularly could contribute to your risks of gaining weight. You can’t understate the social influence. Overall, the BPS model tells us we should consider numerous factors when planning a strategy for good health, rather than focusing solely on biological mechanisms. After all, it’s all connected.
References:
- WHO: International Classification of Functioning, Disability and Health (ICF) https://www.who.int/standards/classifications/international-classification-of-functioning-disability-and-health
- WHO: COVID-19 pandemic triggers 25% increase in prevalence of anxiety and depression worldwide
https://www.who.int/news/item/02-03-2022-covid-19-pandemic-triggers-25-increase-in-prevalence-of-anxiety-and-depression-worldwide - NCBI: Psychological Stress and the Human Immune System: A Meta-Analytic Study of 30 Years of Inquiry
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1361287/ - NCBI: The concept of depression as a dysfunction of the immune system
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3002174/
Three Aspects of Health and Healing: The Biopsychosocial Model in Medicine | Department of Surgery
The Biopsychosocial Model: Causes Of Pathological Anxiety
What is Biopsychosocial model – Meaning and definition – Pallipedia





